The current discoveries in immunology showcase the recent developments and their relevance during the upsurge of COVID-19 cases. This treatise describes the development of immunology as a scientific discipline focused on its foundation.
Researches emphasize the role played by immune-responsive cells in combating cancer, viral defense regulation, and novel targeted immunotherapeutic approaches.
So, let us look at these 2021 research outcomes from a broader perspective.
Table of Contents
- Top Immunology News of 2021
- 1. Stem-like T cells may support immunotherapy for the treatment of cancer (USA, Sept 2021)
- 2. Researchers discover a crucial molecule controlling cell function that is essential for regulating immunity (USA, Jan 2021)
- Top Cell Biology News of 2020 – A Round Up
- 3. Understanding a crucial immune cell’s role in cancer immunity (Australia, April 2021)
- 4. Scientists identified that the innate immune system makes the situation significantly severe for COVID-19 (Sweden, Feb 2021)
- 5. Mast cells as precursor cells are activated by allergic stimulation (Sweden, Sept 2021)
- 6. Discovery of immune cells in the lungs enhances virus defense (Switzerland, Jan 2021)
- 7. Children with multisystem inflammatory syndrome MIS-C mount a typical T cell response to COVID (USA, Oct 2021)
- 8. Effective therapeutic potential treatment for chronic viral infections (Australia, Nov 2021)
- 9. Bone marrow is the crucial player required to tackle respiratory infections (UK, Nov 2021)
- 10. Scientists developed a ‘Clock ‘to forecast aging-related chronic diseases and immunological health (USA, July 2021)
- 11. Researchers used a mathematical model to help optimize vaccine development (Spain, Oct 2021)
- The 23 Best & Free Biology Apps (Android) For Students & Teachers
- 12. A novel targeted immunotherapeutic approach to fighting against cancer (USA, March 2021)
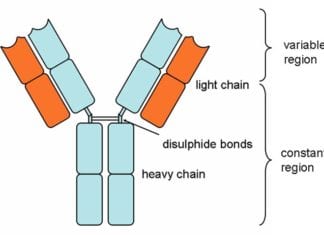
- Explore Types of Antibodies in Blood, Their Structures & Functions
- 13. Researchers have discovered live immune cells in coral and sea anemones (USA, Aug 2021)
- 14. Researchers discover the fuel source that boosts “natural killers” cells in the immune system (USA, June 2021)
- 15. Malaria: New insights regarding acquired immunity may enhance vaccines (Denmark, Nov 2021)
Top Immunology News of 2021
1. Stem-like T cells may support immunotherapy for the treatment of cancer (USA, Sept 2021)
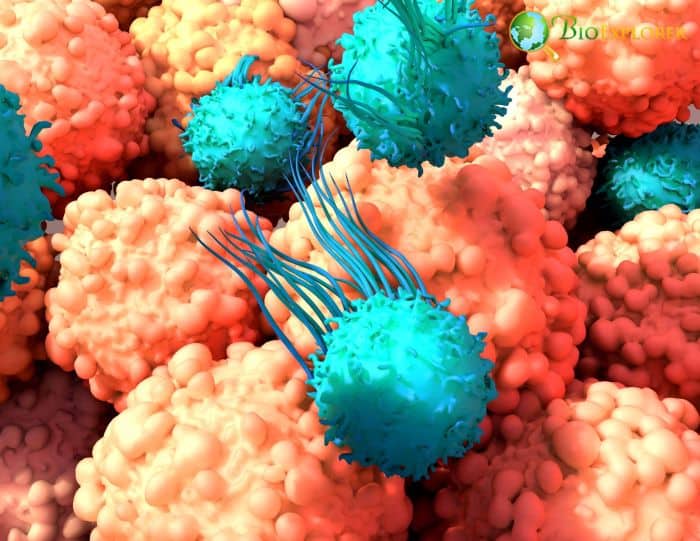
According to research, specific lymph nodes contain stem-like T cells that may act as inborn cancer fighters.
- To examine the stem-like T cells in tumors over several months of tumor growth and determine how the stem-like T cells survive, researchers first created a new animal model.
- They discovered that the stem-like T cells are replenished from another part of the body because they do not stay in the tumor for very long. Instead, the supply was replenished by nearby lymph nodes, an immune organ that houses many of these stem-like T cells.
- A few stem-like T cells occasionally leave the lymph node and move toward the tumor. This continuously supplies the tumor with new cancer-fighting T cells. This, according to researchers, is crucial for containing the spread of cancer.
- During the disease development, stem-like T cells located in the nearby lymph nodes are not exhausted, contrary to our study’s findings about T cells in tumors.
This study focuses on creating treatments that activate the stem-like T cells in the nearby lymph node and use them to combat cancer
Suggested Reading:
Top 15 Immunology News in 2018
![]()
2. Researchers discover a crucial molecule controlling cell function that is essential for regulating immunity (USA, Jan 2021)
Numerous molecules in our bodies support the immune system in keeping us healthy without triggering an excessive immune response that leads to diseases like autoimmune disorders.
- The innate immunity or defense system that has been in place since birth to combat pathogens and keep us healthy includes one molecule called Absent In Melanoma 2 (AIM2). However, little was known about AIM2’s role in T cell adaptive immunity; the body’s defenses that evolved in response to specific pathogens and health issues accrued throughout life.
- AIM2 is crucial for adequately operating regulatory T cells or Treg cells and is critical in preventing autoimmune disease. Treg cells are a fundamental subset of adaptive immune cells that suppresses overactive immune reactions, like those seen in autoimmune diseases.
- Both innate and adaptive immunity carry out typical immune reactions to combat pathogens and preserve biological stability. However, these reactions must be controlled to prevent them from intensifying and leading to a wide range of additional health issues in addition to those the pathogen initially caused.
- Different cell types and molecules have different functions in suppressing innate and adaptive immunity. This research demonstrates that one of them is AIM2 in Treg cells. Treg cells are essential for the immune system’s maintain the homeostatic balance of the immunity system.
Therefore, this suggests a significant function for AIM2 in Treg cells. The AIM2-RACK1-PP2A-AKT pathway is a new cellular signaling pathway of protein molecules in Treg cells. This pathway controls the metabolism and function of Treg cells to prevent autoimmune disease.
Suggested Reading:
Top Cell Biology News of 2020 – A Round Up
![]()
3. Understanding a crucial immune cell’s role in cancer immunity (Australia, April 2021)

A crucial immune function that contributes to the prevention and treatment of cancer and infectious diseases has been identified by researchers as part of the differentiation process.
- According to the research, a new factor called DC-SCRIPT is necessary for the function of a specific class of dendritic cells called cDC1, which is crucial for regulating the immune response to infection.
- Dendritic cells are immune cells that activate “killer” T cells, essential for eradicating viral infections and inciting a response to cancerous tumors.
- Researchers are working to better understand how this process operates to help the body produce many dendritic cells to combat cancer and infections. Enhanced expression of cdcs will increase the body’s normal response to tumors.
Finally, scientists can figure out how to make the body produce many dendritic cells to combat infections and cancer.
Suggested Reading:
Top 25 Immune System Fun Facts
![]()
4. Scientists identified that the innate immune system makes the situation significantly severe for COVID-19 (Sweden, Feb 2021)

The innate immune system overreacts in patients with severe COVID-19. This innate immune system overreacts in patients with severe COVID-19. According to a recent study, this overreaction may be what causes the blood clots to form and the patient’s oxygen saturation to decline.
- Multiple proteins in the blood act as the body’s primary defense against microorganisms, including SARS-CoV-2, by recognizing and destroying them (the virus that causes COVID-19).
- These proteins are a component of the intravascular innate immune system (IIIS), including platelets and specific white blood cells. They are grouped in the blood’s cascade systems. Only 5% of animal species alive today have an immune system with T cells and B cells; the rest exclusively rely on the natural immune system, primarily the IIIS.
- The IIIS functions as a waste disposal system thanks to its innate ability to identify and remove foreign substances and particles, including microorganisms and damaged cells.
- Thereby, it may be concluded that the intravascular innate immune system (IIIS) behaves in this way in some COVID-19 patients may be due to the severity of the cell damage, which causes the IIIS to overreact and create havoc on the tissue rather than clearing it out.
Therefore, from a therapeutic perspective, it can be said that to treat severe COVID-19 with medications already approved for treating hereditary angioedema if the IIIS plays the role that the researchers believe it does.
Suggested Reading:
Explore The Cells of The Epidermis
![]()
5. Mast cells as precursor cells are activated by allergic stimulation (Sweden, Sept 2021)
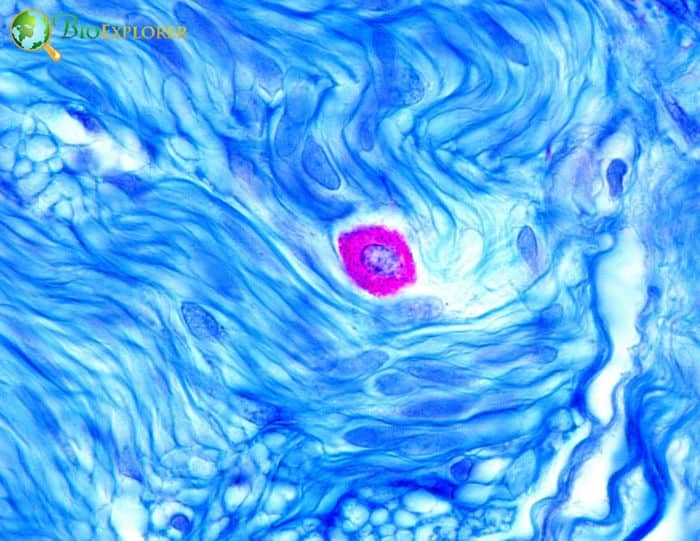
According to a recent study, mast cell precursor cells contribute to an increase in mature mast cells during inflammation and actively participate in diseases like asthma.
- Mast cells are a subset of immune cells only found in tissues that have direct contact with the outside world, like the skin and airways.
- In contrast to other immune cells, Mast cells are created from precursor cells that move to the tissues through the blood. Mast cells express the high-affinity receptor for IgE, the primary antibody linked to allergic reactions, which has a negative impact on the development of asthma and allergies.
- When IgE bound to IgE receptors binds to allergens, substances that cause physiological reactions, such as the contraction of the airways in allergic asthma, are released, activating mast cells.
In healthy individuals, mast cell precursors are uncommon. Still, their frequency rises during inflammation, leading to an increase in mature mast cells. In addition, mast cell growth is well known to be associated with various inflammatory diseases.
Suggested Reading:
Top 10 Discoveries in Immunology 2019
![]()
6. Discovery of immune cells in the lungs enhances virus defense (Switzerland, Jan 2021)

Under the guidance of Professor Carolyn King, researchers from the University of Basel’s Department of Biomedicine have discovered various immune cells in the lungs that are essential for the body’s defense against flu virus reinfection. The possibility of reinfection by different respiratory disease-causing pathogens exists.
- People started to wonder how long immunity lasts after surviving SARS-CoV-2 at the onset of the coronavirus pandemic. Likewise, the COVID-19 vaccination is currently the subject of the same question.
- Immunological memory plays a significant part in this process, a complex interplay of immune cells, antibodies, and signaling molecules that enables the body to effectively combat known pathogens. The study talks about two kinds of T helper cells in the lungs. In the event of reinfection, one type releases signaling molecules to arm other immune cells with more lethal “weapons” to combat the pathogen.
- The other type supports antibody-producing immune cells (B cells) and localizes closely in the lung. Previously, it was thought this type was only present in lymphatic tissue and absent from lung tissue.
- Researchers were able to establish that having these cells nearby the antibody-producing B cells made the immune response to a different flu virus more effective.
The discovery might lead to ways to develop vaccines against rapidly mutating viruses that last longer.
Suggested Reading:
How Do Viruses Reproduce?
![]()
7. Children with multisystem inflammatory syndrome MIS-C mount a typical T cell response to COVID (USA, Oct 2021)
According to a recent study, the rare condition known as a multisystem inflammatory syndrome in children (MIS-C), which is linked to COVID-19, is not brought on by the COVID-19 virus as was previously believed.
- A recent COVID-19 infection is a risk factor for multisystem inflammatory syndrome in children (MIS-C). However, the syndrome is uncommon, and it’s still unknown how the viral infection causes MIS-C or why it only manifests in some kids.
- To address these queries, scientists believe that children with MIS-C might mount an abnormal immune response to the coronavirus via their T cells, which aid the body in fighting viral infections and result in inflammation. But MIS-C does not seem to be caused by abnormal T cell responses to the virus.
- According to the Centers for Disease Control and Prevention, the right approach for parents to protect their children from MIS-C is to take precautions against the household infecting the virus that causes COVID-19, such as masking, avoiding crowded places, and vaccination for those who are eligible.
So, it can be concluded that children with SARS-CoV-2 infection who later developed MIS-C displayed various T-cell response patterns to SARS-CoV-2 peptide epitopes.
![]()
According to a recent mouse model, early activation of the B cell-specific Moloney murine leukemia virus integration site 1 (BMI1protein) BMI-1 in B cells during chronic viral infection disturbs the delicate balance of gene expression, producing antibodies that are unable to eradicate the virus from the body.
- Global health is severely harmed by chronic infectious diseases. An individual’s B cells get altered when ones possess a chronic viral infection like HIV or hepatitis C, which results in weak antibodies that are unable to aid the body in eradicating the infection.
- WhenBMI-1 protein is targeted, the B cell’s nature can be altered to produce an antibody of higher quality that clears viruses faster. This may also open up a new therapeutic pathway to help improve and regulate the antibody response for better results.
- B cells react to infections and potentially develop into plasma cells. The plasma cells are the ones that produce and secrete antibodies. Some activated B cells during an infection can quickly develop into plasma cells and produce antibodies within the first few days of the body’s immune response.
So, working on delivering drugs directly to B cells to improve the antibody response without affecting how well other immune cells work is crucial because memory immune cells and high-quality antibodies are the keystones underlying immune protection provided by successful vaccines.
Suggested Reading:
History of Immunology
![]()
9. Bone marrow is the crucial player required to tackle respiratory infections (UK, Nov 2021)
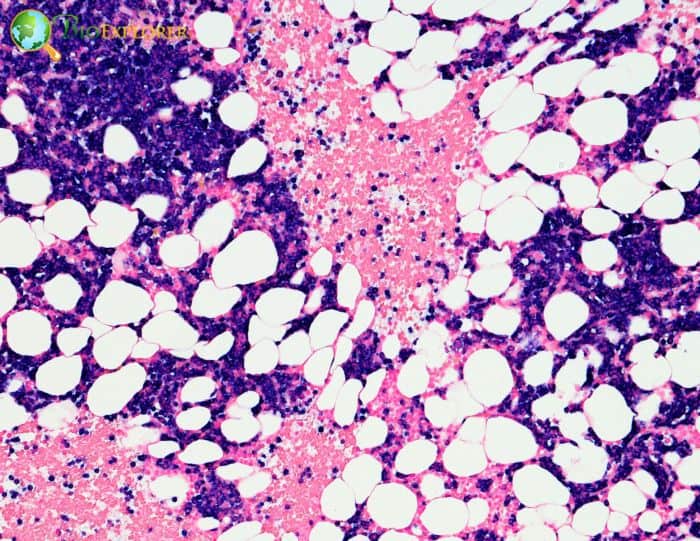
Researchers have discovered how the immune system summons “emergency” dendritic cells in response to an infection, reinforcing the dendritic cells already present at the infection site with new cells that traverse from the bone marrow.
- In the immune system, dendritic cells play a crucial role in detecting pathogenic bacteria, fungi, or viruses that have invaded the body and alerting T cells to identify and combat the invader.
- Dendritic cells in mice infected with the flu virus, which also causes disease in humans, were being watched by researchers. They discovered that new dendritic cells are expelled from the bone marrow and move to the infection site following infection.
- A chemokine receptor type 2 known as CCR2 controls this process by binding chemokine molecules produced by other cells in the infected tissue. The varying concentrations of chemokines that bind to CCR2 in the lung serve as a map to direct the newly formed dendritic cells to the precise location of the virus.
Future treatments and vaccine development for various infectious diseases may benefit from the knowledge of the immune system’s functioning.
Suggested Reading:
Types of Bone Cells
![]()
An inflammatory clock of aging (iAge) that measures inflammatory load and forecasts multi-morbidity, immune health, and cardiovascular aging is also linked to exceptional longevity in centenarians and has been identified by researchers.
- Researchers have identified a small immune protein that plays a role in age-related systemic chronic inflammation and cardiac aging. We currently have tools for spotting dysfunction and a method for intervening before full-blown pathology develops.
- According to the study, the most vital factor influencing iAge is the soluble chemokine CXCL9. According to Furman, that is typically activated to draw lymphocytes to the site of an infection.
- However, in this instance, it is demonstrated that CXCL9 upregulates multiple genes associated with inflammation and is involved in cellular senescence, vascular aging, and adverse cardiac remodeling; it was further observed that silencing CXCL9 reversed loss of function in aging endothelial cells in both humans and mice.
So, with the help of iAge technology, it’s possible to predict chronic systemic inflammation resulting in various diseases seven years in advance.
Suggested Reading:
Top 25 Circulatory System Fun Facts
![]()
11. Researchers used a mathematical model to help optimize vaccine development (Spain, Oct 2021)

A mathematical model is being used by researchers to better understand how the immune system reacts to vaccinations.
- Researchers used a mathematical model to better comprehend the immune response to vaccinations. This might aid in enhancing vaccine design and streamlining related technical difficulties.
- To multiply, viruses are intracellular parasites that depend on host cells. As a result, a virus needs to gain access to some of the body’s cells to grow exponentially before it can infect a person. Within the infected cells, progeny viruses will assemble and, when released, will infect nearby target cells.
- Without an immune reaction to fight the virus, it will continue to spread and potentially harm organs. So researchers used a mathematical model to better understand the immune system’s response to vaccinations.
- This might facilitate vaccine design improvement and simplify related technical challenges. In addition, the use of vaccines can produce antibodies that aid in the neutralization of assembled free viruses and virus-specific cytotoxic T cells that kill infected cells, thereby lowering the number of virus-producing cells.
This mathematical model will give a deep insight into vaccine design and its possible interactions.
Suggested Reading:
The 23 Best & Free Biology Apps (Android) For Students & Teachers
![]()
12. A novel targeted immunotherapeutic approach to fighting against cancer (USA, March 2021)

Researchers developed a novel targeted immunotherapy that targets cancers using new antibodies against genetically altered proteins to combat cancer.
- The researchers’ immunotherapy strategy targets the p53 tumor suppressor gene, the RAS tumor-promoting oncogene, and the T-cell receptor genes.
- The treatment was also examined on cancer cells in a lab and animal tumor models. Bispecific antibodies and Chimeric antigen receptor CAR T cells, which kill both normal and malignant B cells, have proven effective in immunotherapies for B cell lymphomas.
- The fact that humans can tolerate the loss of healthy B cells makes these B cell-targeting therapies effective.
- However, a treatment strategy that eliminates both healthy and cancerous T cells would not be effective in patients with T-cell cancer because healthy T cells are essential for a healthy human immune system.
This immunotherapeutic approach and the development of bispecific antibodies can target different cancer.
Suggested Reading:
Explore Types of Antibodies in Blood, Their Structures & Functions
![]()
13. Researchers have discovered live immune cells in coral and sea anemones (USA, Aug 2021)

A recent study reveals the specialized immune cells in coral and sea anemones. The results are crucial in understanding how corals protect themselves from bacteria, viruses, and other foreign invaders.
- The researchers exposed foreign substances like bacteria, fungal antigens, and beads into a cauliflower coral (Pocillopora damicornis) and starlet sea Anemone (Nematostella vectensis) in the laboratory to discover these specialized immune cells.
- After that, they separated various cell populations using fluorescence-activated cell sorting. Finally, they discovered that specialized cells called phagocytic cells engulfed the foreign particles.
- In contrast, phagosomes, tiny, fluid-filled structures within the cells, worked to eliminate invaders and their own damaged cells.
As the climate change crisis dramatically reduces coral reef biomass and diversity worldwide, a better understanding of how coral cells carry out specialized functions like fighting infections. The findings can aid in creating diagnostic tools for evaluating coral health and diversity.
Suggested Reading:
16 Immortal Animals Who Defy Death
![]()
14. Researchers discover the fuel source that boosts “natural killers” cells in the immune system (USA, June 2021)
Natural killer (NK) cells are allies in the fight against infections and cancer, which are being better understood by scientists.
- Aerobic glycolysis is essential for the protective actions of T cells. However, whether NK cells rely on this metabolism to fuel their activities was unknown.
- Instead of in a petri dish, they could study the metabolism of NK cells in living animals and compare it to the metabolism of T cells in the environment.
- They discovered that about five days before T cells respond with their glycolytic surge, NK cells increase aerobic glycolysis. So it’s essential to keep the speed and responsiveness of these NK cells because they serve as the paramedics of our immune system.
The research has implications for ongoing initiatives to use NK cells as immunotherapy in patients with cancer and other diseases. In addition, they have implications for using NK cells in cell therapy, which involves growing cells outside of patients and then re-injecting them into their blood.
Suggested Reading:
Top 12 Immunology News In 2017
![]()
15. Malaria: New insights regarding acquired immunity may enhance vaccines (Denmark, Nov 2021)

The body employs a more effective defense when one develops immunity to malaria after acquiring the illness than if one had received a malaria vaccination. Therefore, the researchers believe new findings could enhance malaria vaccines.
- The immune system can activate various defense mechanisms to protect the body. For example, macrophages are the body’s typical line of defense against infections with parasites, viruses, and bacteria.
- Researchers have found that how immunity to malaria appears to function varies. Here, additional cell types are utilized by the body’s immune system to combat infection with the malaria parasite.
- According to whether you were immunized or infected, we’ve discovered that the antibodies have different appearances. As a result, the body employs what is known as natural killer cells as a different form of defense.
- Researchers typically recognize natural killer cells as one of the body’s most effective tools for combating cancer cells. However, it now appears that the immune system that fights cancer and defense against malaria.
- The immune system is better equipped to fight malaria than other common infections. Perhaps because it is such a contagious and fatal disease, it has evolved in this way.
Recent research suggests a fresh approach to creating future malaria vaccines that are even more effective. Because vaccines can be used to mimic how the body mobilizes its defenses with natural killer cells.
Suggested Reading:
Top 10 Immunology News of 2020
![]()
This immunology news gives us a broad overview of the recent advancement in this field. During the epidemic with the upsurge of COVID cases, there have also been researched and developments in this area with the concept of T-cells, natural killers to novel therapeutic approaches of immunotherapy, viral defense, the understanding role of the immune response against cancer and various chronic inflammatory diseases.
Through these scientific interventions and discoveries, we look forward to more exciting findings in 2022.
![]()