
The immune system is one of the most complex and multi-layered systems of our body. We depend on it to fight various types of infections, eliminate dead cells, and fight cancer.
Unfortunately, pathogens and cancer cells can use the immune mechanisms to their advantage or suppress them – that is why we get sick.
The immune system can also become disbalances, leading to autoimmunity and allergy. Thus, understanding the immune system better has become crucial while fighting the current pandemic. Researchers study how the SARS-Cov2 circumvents the immune system’s power to counteract its influence.
Table of Contents
- Immunology News of 2020
- 1. I am a lymphocyte, and I am digging a tunnel – Immune cells can dig tunnels in the extracellular matrix – [Germany, December 2020].
- 2. The T-cell that brings hope: a new type of immune cell ideal for cancer immunotherapy discovered – [UK, January 2020].
- 3. COVID-19 weaves a complex web of interference: SARS-COV2 can block protein production in the cell on several levels, a study finds – [USA, October 2020].
- 4. Follow the light: a new synthetic gene activator switched on by light can be used to guide cancer immunotherapy – [USA, February 2020].
- 5. A new parasite-destroying antibody found in malaria-resistant children: recent research provides a new idea for a vaccine against malaria- [USA, April 2020].
- 6. Tuberculosis bacterium is a professional sabotage agent: tuberculosis infection blocks energy production in immune cells study finds – [Ireland, January 2020].
- 7. Breast cancer cells sabotage immunity – study finds – USA, July 2020.
- 8. Men are from Mars and have unique immune system features – male adipose tissue contains a type of cell that makes them susceptible to metabolic disorders through the immune system – [Australia, February- 2020].
- 9. Hiding weapons of destruction against COVID-19 – highly potent antibodies against SARS-COV2 found – [USA, July 2020].
- 10. Not only vertebrates: insects can inherit protection against viruses, a study finds – [France, 2020].
Immunology News of 2020
While COVID-19 is a most urgent threat currently, other severe infections, such as malaria and tuberculosis, remain still prevalent – and the answers to eliminating them may also lie within our understanding of the immune system.
That is why the research done in 2020 is so vital for healthcare worldwide, as it covers multiple vital issues.
1. I am a lymphocyte, and I am digging a tunnel – Immune cells can dig tunnels in the extracellular matrix – [Germany, December 2020].
Cytotoxic lymphocytes[1] are immune cells that can recognize damaged, dead, or dangerous cells and kill them. They can move around inside the tissues to look out for their potential targets.
Cytotoxic lymphocytes or CTLs are crucial in fighting the immune system against cancer.
Unfortunately, cancer tumors do their best to prevent the attack of CTLs. In addition, they do their best to become inaccessible to the killer cells. To outsmart them, it is crucial to understand how CTLs actually get around the tissues and what influences their efficiency.
A team at the University of Saarland has decided to re-create the environment the CTLs would find themselves in tissues to understand how they move there. The space between the cells in a tissue is usually filled by the extracellular matrix[2]. Each tissue has its own type of extracellular matrix or ECM. Still, some components are standard for all such structures – for example, collagen.
Knowing this, the researchers have built several networks based on bovine collagen. Each imitation matrix had a different collagen concentration.
Then they let the lymphocyte inside their “artificial ECMs” and observed the changes in ECM and cells with the help of light-sheet microscopy. They have discovered that:
- CTLs can move inside the ECM with different speeds – slow, fast, and mixed.
- CTLs use cellular projections to push away the collagen fibers during slow motion, creating a tunnel.
- Other cells can follow the “digger cell“, and they would move significantly faster.
- Cells can switch between those modes of movement.
- Therefore, the efficacy of CTL activity could be significantly influenced by the quality of the channel network present in a particular tissue.
- It is known that cancer tumors have very dense ECMs that can make them resistant to therapy[3].
- A better understanding of these processes can contribute to better cancer therapy in the future.
![]()
2. The T-cell that brings hope: a new type of immune cell ideal for cancer immunotherapy discovered – [UK, January 2020].
Immunotherapy[4] is a recently introduced type of treatment for cancer. This type of therapy uses modified immune cells, called CAR T-Cells[5], specifically tuned to a patient and can find and kill cells of the patient’s specific type of cancer.
The plus side of this approach is that the patient’s cells are used. If the cell engineering is done correctly, only the cancer cells are killed without significant damage to the body’s normal cells.
But, unfortunately, this type of therapy has its drawbacks as well:
- The T-cells must identify cells with a specific protein on their surface. If the cancer cells hide their identification, a T – cell would either not find it or attack a normal cell instead.
- Most T-cells used in therapy rely on a specific marker protein called MHC[6].
- MHC is highly variable and is basically used as a code to determine the body’s cells from the invading cell.
- Therefore, it is hard to program T-cells’ specificity that would be aimed against tumors relying only on MHC molecules.
The research team at Cardiff University has decided to look into circumventing the poor efficacy of using MHC proteins. To do this, the researchers:
- Have undertaken a genome-wide screening of immune cells.
- They have found a group of T cells that have a receptor to another marker protein – MR1.
- When T-cells carrying MR1 were cultured in the dish with different cancer cells, they effectively killed them.
- When the new type of MR1-based T cells was tested in mouse cancer models, the tumors in mice decreased without complications for the animals themselves.
This discovery could radically change cancer treatment, as new types of cells were effective against various cancer types.
![]()
3. COVID-19 weaves a complex web of interference: SARS-COV2 can block protein production in the cell on several levels, a study finds – [USA, October 2020].

One of the principal instruments in the immune system’s fight against viruses is the production of interferons[7]. Interferons can be produced by immune cells and other body cells.
These proteins suppress the production of new viral particles and activate multiple mechanisms involved in the antiviral defense. In their turn, viruses also evolve mechanisms to block interferon production and continue their activity.
The new SARS-COV-2 virus, or COVID19, has spread worldwide since December 2019. Therefore, it is crucial to understand how it evades the immune system and kills people so efficiently.
Notably, it was discovered that this virus could block the production of antiviral interferons altogether in case of the severe course of the infection[8]. A collaboration between the research teams at Caltech and the University of Vermont has helped to explain how:
- The research team proposed that the ability of the COVID-19 virus to block reactions within the cell could probably be explained by the interactions of its proteins with mRNA[9].
- mRNA is a crucial molecule in the cell – it carries the copies of instructions from genes used to make proteins.
- In normal circumstances, a newly made mRNA would pass the following steps:
- Parts of the mRNA would be cut out to make a comprehensible “protein recipe“.
- mRNA attaches itself to a particular structure called a ribosome.
- While mRNA is attached to a ribosome, it produces a new protein.
- It was found that components of the SARS-COV2 virus interfere with all these steps.
- One protein prevents splicing of mRNA, while others interfere with the attachment of mRNAs to Ribosomes and prevent protein production.
- By blocking these steps, the virus prevents the production of most proteins that can potentially harm it by switching on the immune response.
- As the researchers tested only individual proteins of the virus in uninfected cells, they could not predict the possible ways the presence of all viral proteins during the infection would influence the activity of cells in the body of the infected patient.
- This work has two significant advantages:
- It showcases some of the critical mechanisms that cause damage to the infected patient.
- It also shows the possible approach to studying the mechanism of the virus by investigating how viral components interact with the RNAs of the cell.
Knowing mechanisms that the virus employs to promote infection can potentially help develop medication against the coronavirus infection.
![]()
4. Follow the light: a new synthetic gene activator switched on by light can be used to guide cancer immunotherapy – [USA, February 2020].
As mentioned earlier, a CAR T-cell is a type of cell taken from a cancer patient and changed so it can attack a cancer cell specifically. Currently, CAR T-cell immunotherapies are effective in a small number of blood cancers.
One of the reasons for this is that the manipulated immune cell can potentially attack a normal cell instead of the cancerous one. Researchers try out new approaches that would make immunotherapies capable of attacking solid tumors safely as well.
A research team from the University of California San Diego[10] proposed its own version of CAR T-cell therapy:
- The researchers have developed a unique light-switch system called LINTAD to be integrated into the engineered T cells.
- This system can regulate the genes of choice within the cell.
- This switch system was first successfully tested in kidney cell culture.
- The system was also tested in the Jurkat T cell line.
- The light could switch on the required genes in all these cases, while the absence of light stimulation quickly stops the gene activation.
- The engineered T cells were combined with the Non-Hodgkin lymphoma cell culture.
- The cancer cells in this culture had a protein called CD19 on their surface.
- When the engineered cells were stimulated with blue light, they could recognize the CD19 antigen and bind to it.
- When cells were injected with regulator elements containing LINTAD, they could also kill cancer cells upon stimulation.
This new method provides safe, non-invasive regulation of engineered immune cells and can ensure the targeted killing of cancer cells. However, as this regulation is light-dependent, this therapy could only potentially be used for tumors close to the skin.
![]()
5. A new parasite-destroying antibody found in malaria-resistant children: recent research provides a new idea for a vaccine against malaria- [USA, April 2020].
Malaria[11] is a dangerous infectious disease caused by an intracellular parasite, Plasmodium falciparum[12]. Although malaria has been a threat for centuries and a focus of research for many health professionals, there are still very few options for prophylaxis and treatment in the countries where this disease is still prevalent.
One of the possibly promising approaches to counteract the spread of malaria is vaccine development. Unfortunately, malaria is caused by a relatively big, eukaryotic organism with a complex lifecycle, so choosing a target for a future vaccine is hard.
Most vaccines are based on antibodies[13] – proteins produced by immune cells that attach to the pathogen’s corresponding proteins. By providing additional ready-made antibodies, the vaccine helps meet the attacking infection agent upon entry, preventing disease development. Such antibodies can be found in the blood of organisms that have learned to resist the infection by themselves.
To find an antibody that could potentially protect one from malaria infection, a group of researchers has undertaken a long-term study in mothers and children in Tanzania[14].
For this study, 453 children were followed up since birth to register the possible appearance of either malaria infection or resistance to malaria with time. More than 10 years have passed since the start of this study.
As the result of the initial analysis, the researchers have found children resistant to malaria and stored the blood plasma obtained from them. Currently, the new methods of analysis have allowed them to carry out a new set of experiments:
- The researchers pooled all the plasma obtained from children with resistance to malaria infection.
- The scientists acted based on the assumption that the plasma of resistant children would contain antibodies to malaria agent proteins.
- The team then used the plasma together with P. falciparum cultures in a series of so-called biopanning experiments[15].
- These experiments involve testing the parasite’s genes and finding if there are corresponding antibodies to their products in the plasma of resistant people.
- After extensive analysis, the team has focused on the gene called PfGARP . .
- This gene has several valuable features that make it a likely target for a vaccine:
- This gene is present only in species of Plasmodium most likely to cause malaria.
- This gene is also unique to the Plasmodium genus and is not found in other organisms studied to date.
- There is no structure overlap with other proteins belonging to the parasite or the human host.
- PfGARP is active only on a particular stage of the Plasmodium life cycle – the trophozoite form that develops inside the infected erythrocyte[16].
- If the parasites are subjected to the anti – PfGARP antibody, they stop growing and die.
- All the features listed above make the anti-PfGARP antibody a reasonable basis for an antimalaria vaccine.
Suggested Reading:
Top 25 Endocrine System Fun Facts
![]()
6. Tuberculosis bacterium is a professional sabotage agent: tuberculosis infection blocks energy production in immune cells study finds – [Ireland, January 2020].

Tuberculosis[17] is one of the infectious diseases that were consistently hard to conquer for several centuries. The microorganism causing tuberculosis, Mycobacterium tuberculosis[18], is currently resistant to many antibiotics and is very hard to treat.
Moreover, this bacterium also negatively affects the patient’s immune system.
A team of scientists at Trinity College, Dublin, has studied the influence of Mycobacterium tuberculosis on one of the crucial types of immune cells – macrophages[19]:
- Scientists have compared the effect of heat-killed mycobacteria and live mycobacteria on macrophages.
- To produce immunoreactive substances necessary for immune defense, macrophages rely on a biochemical process called glycolysis[20].
- Glycolysis is a crucial stage that provides necessary materials for energy production in the mitochondria of the cells.
- It was discovered that when macrophages were cultured with dead bacteria, the process of glycolysis was normal.
- Macrophages interacting with living M. tuberculosis had disrupted the glycolysis process.
- The disruption in the glycolysis reactions was caused by the small RNA molecule called mIR-21.
- mIR – 21 blocks the production of the protein PFK-M.
- PFK-M is an essential component of the glycolysis process.
- It was found that blocking the activity of mycobacterial mIR-21 could re-activate glycolysis in macrophages.
- In typically active cells, macrophages can produce IL-1β, an immune protein that blocks M. tuberculosis growth.
- In cells with blocked glycolysis, no IL-1β gets produced.
- If the mIR-21 is blocked, the cells can produce more necessary proteins.
This discovery explains one of the essential aspects of the M. tuberculosis infection. Furthermore, it shows a potential approach to the treatment of tuberculosis.
![]()
7. Breast cancer cells sabotage immunity – study finds – USA, July 2020.
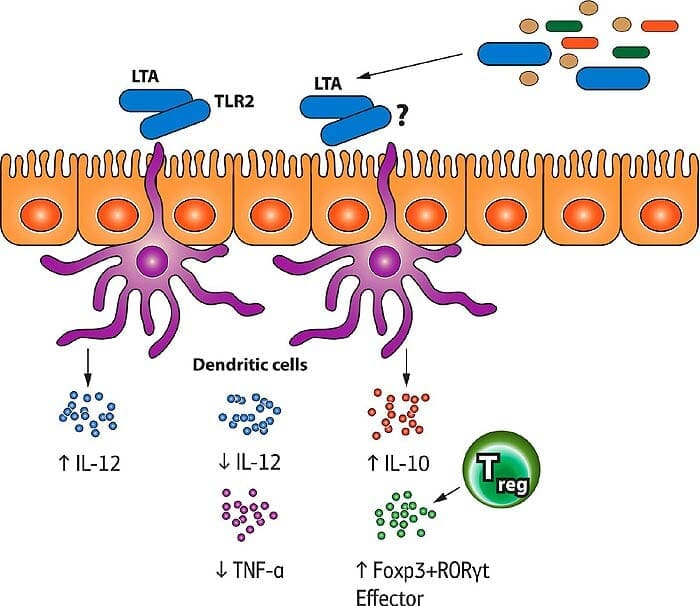
One of the immune system’s jobs is to identify cancer cells in advance and kill them. This essential patrol duty is called immune surveillance[21].
During immune surveillance, a particular subdivision of immune cells called antigen-presenting cells find potentially harmful cells, destroy them, and use proteins from the destroyed cells to activate other immune cells that can mount a final blow, usually T lymphocytes.
Unfortunately, this mechanism is not entirely effective. Tumor cells have a mechanism that allows them to evade immune system activity.
Some tumor cells just do not have the proper signals that could help identify them – therefore, they are simply not “seen” by the cell guards.
Other cells produce molecules that decrease the efficacy of immune killer cells against cancer. Recently, a group of researchers from Cold Spring Harbor Laboratory[22] has identified the third cancer defense mechanism. This mechanism influences a crucial subset of immune cells – dendritic cells[23].
These cells mediate between other immune cell types, showing them the potential “enemy” markers. The researchers have found the following:
- In breast cancer tumors with a unique marker called CCR2, tumors grow faster.
- If the tumor cells lack this marker, the tumor grows significantly slower.
- If the tumor cells have no CCR2 or this marker is blocked by antibodies, the tumor gets surrounded by several types of immune cells.
- Immune cells help shrink the tumor.
- Previously, it was thought that CCR2’s primary function was to guide immune cells to areas with inflammation[24].
- The new study found that CCR2 in breast cancer tumors prevents dendritic cells from reaching maturity.
- If dendritic cells mature correctly, they can attract multiple killer cells toward the tumor.
- Therefore, blocking CCR2 in tumors can help destroy cancer with the patient’s own immune system.
This discovery is a double breakthrough. First, a new important function for CCR2 was discovered. Second, a new potential line of treatment has opened up. However, it would need multiple studies to achieve a harmless CCR2 block, as this molecule is still vital for immunity in normal conditions.
![]()
8. Men are from Mars and have unique immune system features – male adipose tissue contains a type of cell that makes them susceptible to metabolic disorders through the immune system – [Australia, February- 2020].

Obesity is currently a global problem. However, few people realize that obesity can be linked to different problems, from diabetes to autoimmune disorders.
Interestingly, there is a clear divide between males and females regarding obesity-related diseases: males are more likely to develop type 2 diabetes[25] and other metabolic disorders, while women are more prone to autoimmunity.
This difference was previously linked to a part of fat tissue called visceral adipose tissue[26]. This part of the body has crucial importance, as the cells in this area produce hormones that influence multiple processes[27].
Two teams of researchers from Doherty Institute and Walter and Eliza Hall Institute have decided to compare the visceral adipose tissue between males and females:
- The researchers have found a new cell type in the male adipose tissue.
- This cell was found to produce a substance called interleukin 33 or alarmin[28].
- Il-33 was previously found to support inflammation[29].
- Alarmin can promote inflammation by influencing immune cells called T regulators[30].
- T regulators are critical immune cells that can limit inflammation or stop it altogether.
- The cells that produce alarmin in male fat tissue are controlled by testosterone.
- Therefore, in certain situations, testosterone production can lead to increased inflammation in the fat tissue.
- In its turn, inflammation in that area is linked to metabolic disorders, including diabetes[31].
This discovery is unique as it shows for the first time that immune cells are directly linked to male hormones’ activity. It is also the first mention of a potentially unique mechanism that contributes to obesity and diabetes in men.
Moreover, it also shows that scientists must evaluate and study fat tissue in both genders separately to understand metabolic disorders better, as they have specific differences.
![]()
9. Hiding weapons of destruction against COVID-19 – highly potent antibodies against SARS-COV2 found – [USA, July 2020].
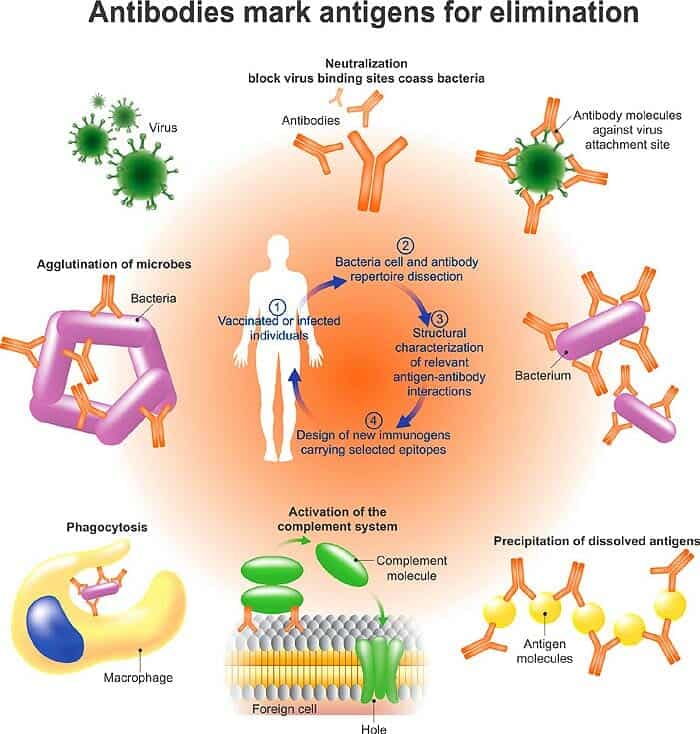
In the absence of either effective vaccines or effective medicines against coronavirus infection, the only hope for treatment lies with the affected patients.
Using plasma from recovered patients was one of the potential treatments against the new infections. It was possible because our bodies produce antibodies that neutralize the invading pathogen during infection, making it easier for the immune cells to destroy them.
The search for the most effective antibodies was actively conducted in 2020 and continues until now. One of the most successful finds was made by the team at the Columbia University Vagelos College of physicians and Surgeons.
The team led by David Ho has studied five patients with severe coronavirus disease:
- The researchers have found 19 antibodies with powerful neutralizing properties against the COVID-19 virus.
- Most of the antibodies could attach themselves to the spike protein[32] of the virus.
- Most importantly, each type of antibody could attach to a different area on a spike protein.
- Some antibodies found could block more than 50% of viral particles in laboratory experiments.
- The antibodies used together can also bind to the spike protein’s “locked down” shape that usually allows the virus to evade the immune system.
This finding is essential as these antibodies can be used both in vaccine development and for therapy COVID19 and can potentially counteract the resistance of new virus variants.
![]()
10. Not only vertebrates: insects can inherit protection against viruses, a study finds – [France, 2020].
One of the crucial differences between vertebrates and invertebrates is the organization of their immune system. In vertebrates, from mammals to other types of animals, two types of immunity are present: non -specific, innate immunity that uses “first responder” cells to stop the attacking pathogen, and adaptive immunity, which mounts a response specifically tailored to pathogens.
Invertebrates have only innate immunity mechanisms. It was previously thought that the innate immunity of insects is not heritable and does not have specific “tailoring” for different pathogens[33].
Recently, the Institute Pasteur team under Maria Carla Saleh’s leadership has found that reactions to pathogens in Drosophila melanogaster flies can differ depending on the type of the agent and the way it has entered the insect’s body[34].
Further experiments have shown some other unexpected findings:
- The researchers infected the fruit fly Drosophila melanogaster with several RNA viruses.
- It was found that the offspring of the flies infected with such viruses could mount a more effective response against the pathogen compared to the parents.
- Similar protection for the next generation was observed in mosquitoes whose parents were previously inoculated with the chikungunya virus.
- Immune reactions were also seen in both types of insects towards artificially made viruses.
- This mechanism of inherited protection functioned only for viruses that consisted only of one strand of RNA.
These findings show the potential mechanism contributing to the tolerance of viruses in the mosquito, a common vector for multiple blood-borne diseases. In addition, this study has also shown for the first time that insects could inherit protection against pathogens from their parents.
![]()
In this new age of the pandemic, immune system studies have become even more crucial than previously. The studies in 2020 have helped us understand better how COVID-19 weakens the immune system[35]. In addition, new mechanisms of antiviral defense[36] were also discovered.
There was also active research devoted to developing vaccines against other diseases, such as malaria vaccine[37] and flu vaccine[38]. In addition, scientists have also better understood other types of immune mechanisms, for instance, protective cells in the brain[39].
New discoveries will likely continue to appear in the immunology field – both in COVID19-related research and in other areas.
![]()


















